An incisional hernia occurs when part of the intestine or abdominal tissue pushes through the abdominal wall at the site of a previous surgical incision.
It often appears as a visible bulge near the old surgical scar, especially when bending, coughing, or lifting something heavy.
In some cases, the bulge may remain visible even while standing or lying down.
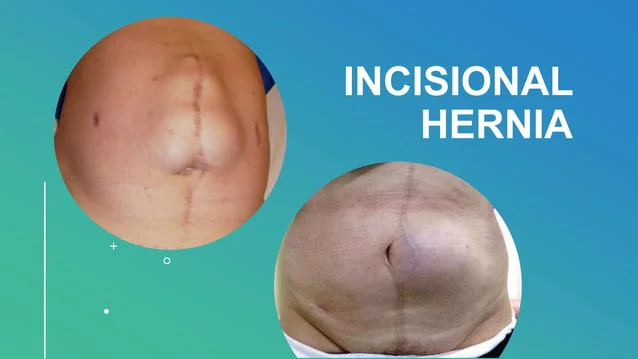
When you have these Warning Symptoms of incisional hernia like:
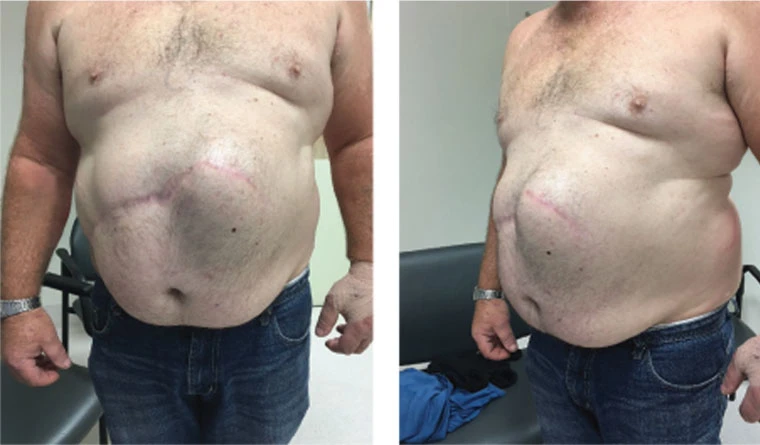
Incisional hernias can develop after open abdominal (laparotomy) or minimally invasive surgeries.
After surgery, the abdominal muscles need time to heal. If they weaken or don’t heal properly, tissues can push through the incision site.
Factors that increase the risk include:
➡️ Around 20% of people who undergo laparotomy may develop an incisional hernia, sometimes months or years after surgery.
Your doctor may recommend:
No. Medicines cannot repair the muscle defect. Since an incisional hernia is a structural problem in the abdominal wall, surgery is the only effective treatment.
Since an incisional hernia is a mechanical defect in the abdominal wall, surgery is the only effective treatment. Medicines cannot repair the muscle gap or push the herniated contents back into the abdomen.
Before surgery, your doctor will evaluate and manage any underlying causes — such as chronic cough, constipation, infection, or obesity — to ensure proper healing and reduce the risk of hernia recurrence after the operation.
The standard surgical procedure for an incisional hernia is a Mesh Repair – open or laparoscopic (keyhole surgery)
During the operation, the surgeon carefully opens the hernia sac, returns the protruding tissues or intestines back into the abdomen, closes the muscle defect, and then reinforces the area with a non-absorbable surgical mesh to provide additional strength and prevent recurrence.
This procedure can be performed either laparoscopically (keyhole surgery) or through open surgery, depending on the size of the hernia, the patient’s medical condition, and the complexity of the case.
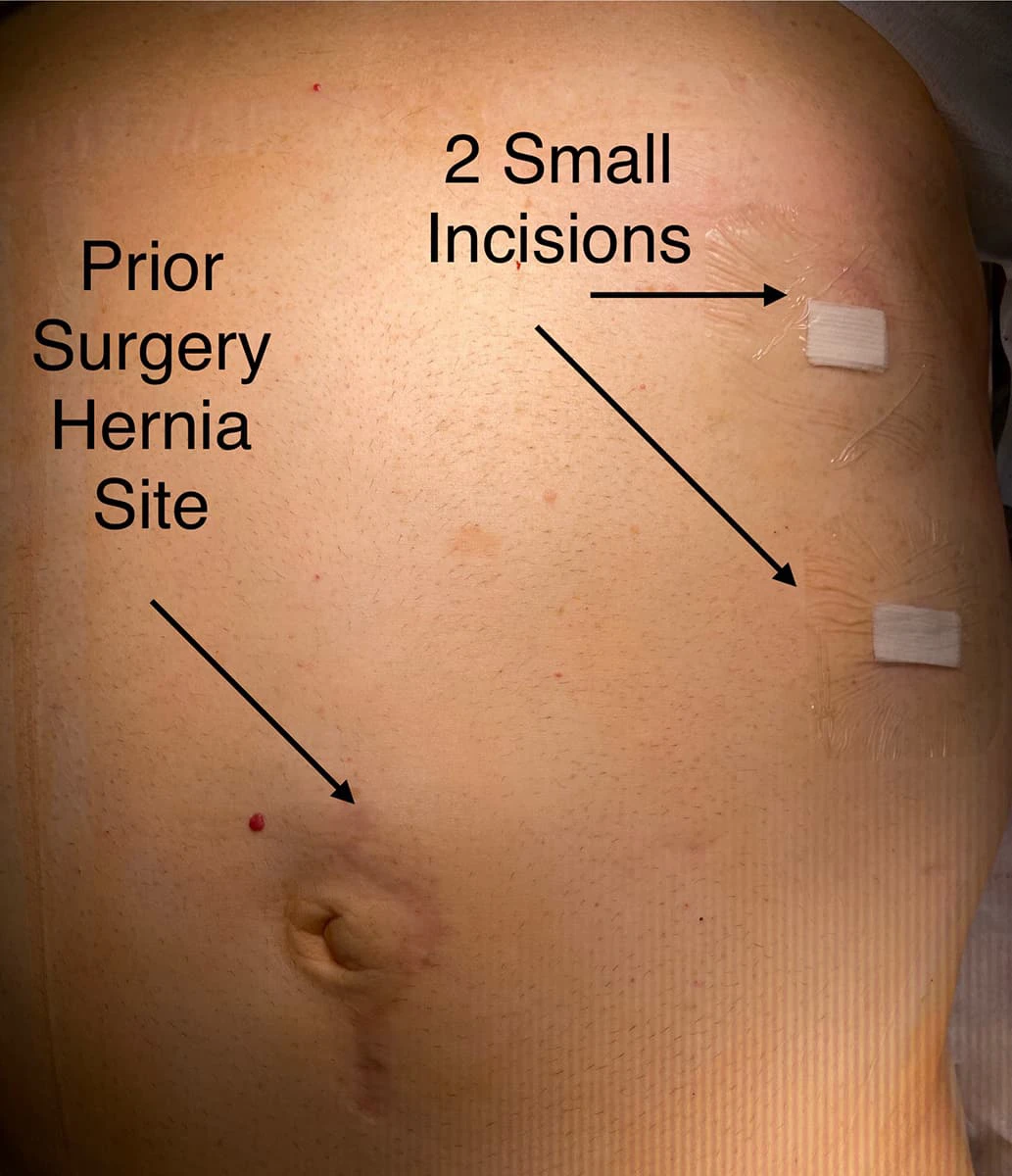
It’s a simple surgery done by using laparoscopy and 3 pin hole incisions(cuts). The hernia is reduced from inside and mesh is placed inside intraperitoneally.
Patients who are medically fit to receive general anaesthesia are good candidates for laparoscopic repair.
Open surgery is recommended in specific situations where laparoscopic repair may not be suitable. These include:
In complicated cases of incisional hernia, where a portion of the intestine becomes trapped (strangulated) and loses its blood supply, emergency surgery is required.
During the procedure, the non-viable (dead) section of the intestine is carefully removed (bowel resection), and the healthy ends are stitched back together to restore normal intestinal continuity.
Prompt medical attention is crucial, as delayed treatment can lead to severe infection, sepsis, or life-threatening complications.
Immediately after surgery:
Long-term care:
Mesh fully integrates into your body in 6–8 months. So, after surgery patients are advised to
Immediately after surgery:
Long-term care:
Mesh fully integrates into your body in 6–8 months. So, after surgery patients are advised to
It can develop months or even years after the original surgery.
Untreated hernias can become irreducible or strangulated, cutting off blood flow to intestines — a life-threatening condition that requires emergency surgery.
No, mesh repair is a routine procedure and not life-threatening in most cases.
Our expert team provides world-class treatment for Incisional Hernias and other gastrointestinal diseases using advanced techniques and compassionate care.
📞 Book your appointment today to consult our specialist gastro for timely diagnosis and treatment.