If you experience persistent upper abdominal pain, especially after meals or with vomiting, consult a surgical gastroenterologist immediately. Early treatment can prevent severe complications.
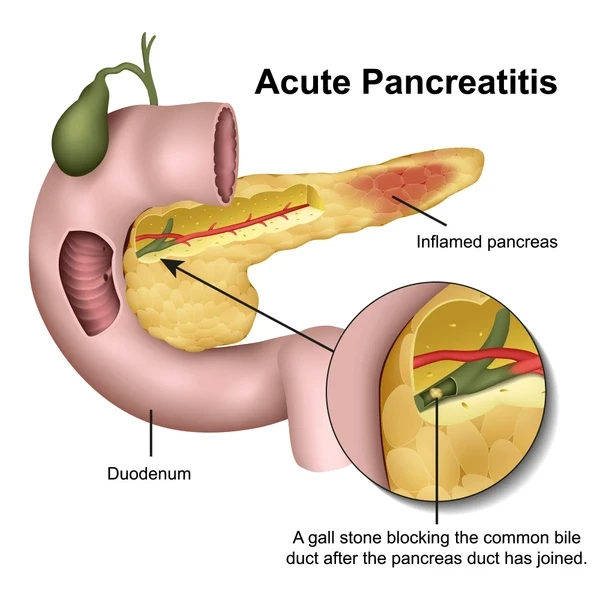
Acute pancreatitis is a sudden inflammation of the pancreas — a vital organ located behind the stomach that helps with digestion and blood sugar regulation. It occurs when digestive enzymes within the pancreas become active too early, causing irritation and inflammation of the organ. It can range from mild pain to a severe, life-threatening condition.
Common symptoms include:
Severe abdominal pain that does not settle is a medical emergency and should be evaluated immediately by a gastroenterologist.
The most common causes are:
In some cases, the exact cause remains unknown (idiopathic pancreatitis).
Diagnosis is based on:
Most cases are treated medically. However, surgery or endoscopic gallstone removal (ERCP) may be needed if:
Most cases are treated medically. However, surgery or endoscopic gallstone removal (ERCP) may be needed if:
Untreated pancreatitis can lead to:
Immediate treatment is essential to prevent complications.
Yes. Recurrence is common, especially if the underlying cause (gallstones, alcohol, metabolic issues) is not treated. Preventive management such as cholecystectomy (gallbladder removal) or lifestyle modifications may be advised.
In severe or recurrent cases, the pancreas may fail to produce enough digestive enzymes, leading to:
Enzyme supplements or long-term management may be required.
If you experience persistent upper abdominal pain, especially after meals or with vomiting, consult a surgical gastroenterologist immediately. Early treatment can prevent severe complications.