An anal fissure is a small crack or tear in the lining of the anal canal. It usually occurs when hard or large stools pass through the anus, causing a tear in the delicate skin and resulting in pain or bleeding during bowel movements.
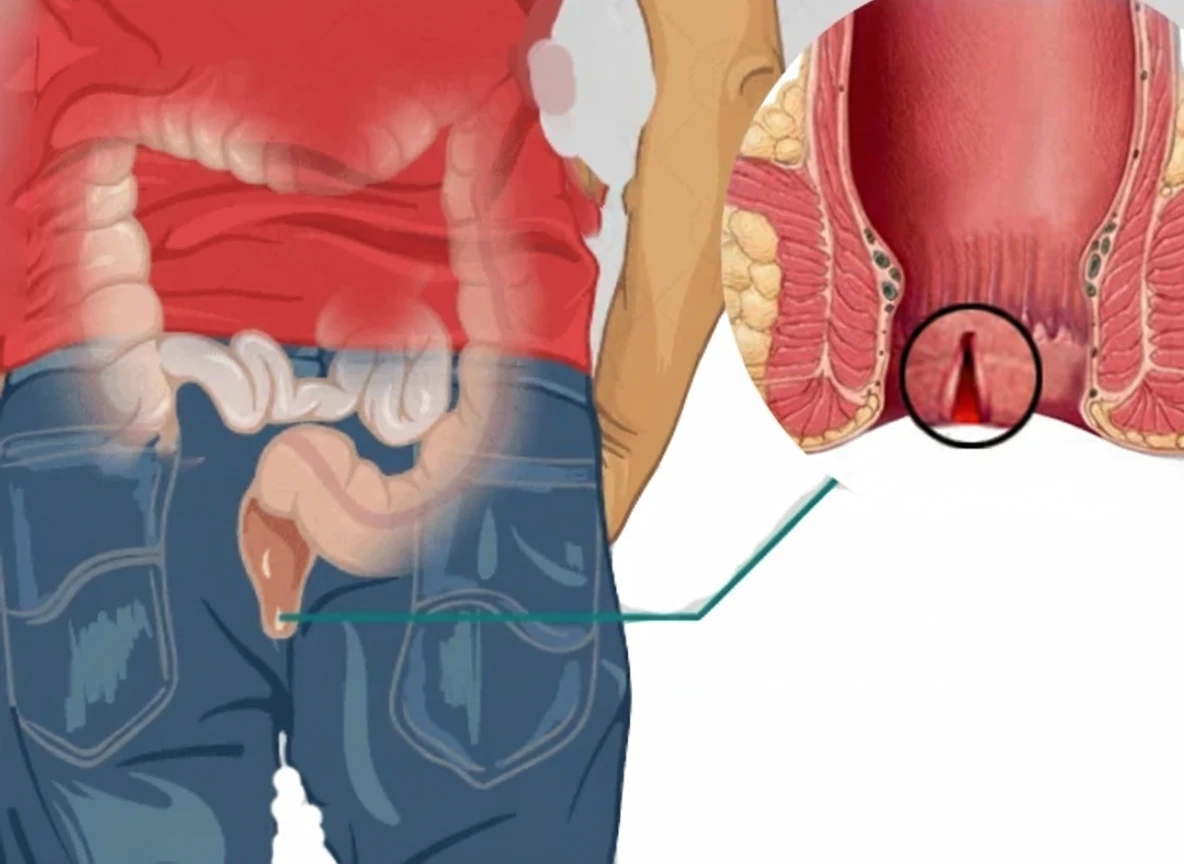
Anal fissures are usually caused by:
In some cases, fissures can occur due to underlying conditions such as:
Diagnosis is made through a clinical examination of the anal area to assess the fissure, its severity, and the presence of any skin tags.
In recurrent or chronic fissures, or when conditions like Crohn’s disease are suspected, doctors may recommend an ileo-colonoscopy for further evaluation.
You should consult a doctor if you experience:
Early treatment helps prevent chronic fissures and complications.
If left untreated, an anal fissure may lead to:
These two conditions are often confused:
Both terminologies are used often and confusingly. Fissure is a split in the lining of anus and is painful. Piles or Hemorrhoids are painless, blood vessels of anal canal which descend down and outside the anus.
In over 99% of cases, anal fissures heal with medical management. Treatment includes:
Avoiding non-vegetarian and spicy foods helps in faster healing.
Surgery is rarely required.
It is considered only in chronic, long-standing, non-healing fissures. The procedure, called Lateral Internal Sphincterotomy (LIS), involves making a small cut in the internal anal sphincter muscle to reduce tension and allow healing.
In chronic fissures, the skin around the anal opening may thicken and form a small lump or skin tag. These are not piles and not cancerous.
Painless skin tags are usually left alone. Small painful skin tags settle down on treatment of the anal fissure.
Very large painful ones need to be surgically excised.
Most acute fissures heal naturally with dietary changes, laxatives, and local creams.
However, if your fissure hasn’t healed within a few weeks, it may be chronic and needs medical or surgical treatment.
Most acute fissures heal within a few days to weeks.Chronic fissures that last more than eight weeks may require treatment, and complete healing can take an additional 6–12 weeks with proper care.
You can prevent fissures by:
Untreated fissures may become chronic and lead to complications such as:
Yes, both stress and diet can indirectly contribute to the development of anal fissures.
When you’re stressed, your digestive system often slows down, leading to constipation and hard stools — the most common triggers for anal fissures. Stress can also tighten the anal sphincter muscles, making bowel movements more painful and increasing the risk of small tears.
A poor diet low in fiber and fluids can make stools hard and difficult to pass, causing strain and injury to the anal lining. Consuming too much spicy, oily, or processed food can further irritate the anal area and worsen symptoms.
To prevent fissures, manage stress through relaxation techniques, stay hydrated, and maintain a fiber-rich diet with plenty of fruits, vegetables, and whole grains.
Home remedies can help heal mild or acute anal fissures, but they may not cure chronic or long-standing fissures permanently.
Simple lifestyle changes like drinking plenty of water, eating a high-fiber diet, and taking sitz baths (sitting in warm water for 10–15 minutes, twice a day) can relieve pain and promote healing. Using stool softeners or natural laxatives like isabgol (psyllium husk) also helps reduce straining during bowel movements.
However, if the fissure has become chronic (lasting more than 6–8 weeks), it may not heal completely with home remedies alone. In such cases, medical treatment — including prescribed ointments that relax the anal sphincter — or minor surgery may be required for permanent relief.
Our expert team provides world-class treatment for Anal Fissures and other gastrointestinal diseases using advanced techniques and compassionate care. We focus on providing lasting relief and promoting healing.
📞 Book your appointment today to consult our specialist gastro for timely diagnosis and treatment of Anal Fissures.